FAQs About Blood Transfusions for CAD
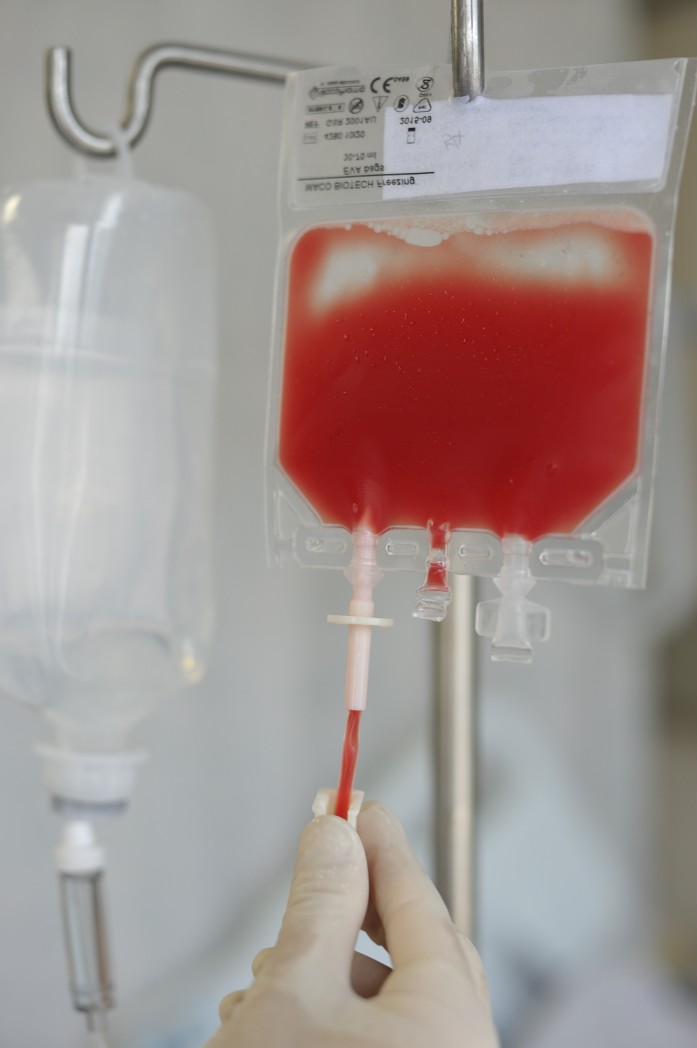
Cold agglutinin disease (CAD) is marked by the destruction of red blood cells, cells essential to transporting oxygen to tissues. Their loss can lead to symptoms that include joint pain, fatigue, and cardiac issues. Your doctor may recommend a blood transfusion to help ease these symptoms.
Here are answers to some frequently asked questions about blood transfusions.
What is a blood transfusion?
A blood transfusion is a process in which you receive blood from a donor intravenously (IV). The most common forms of blood transfusion are red blood cell (the cells that carry oxygen and give blood its color), platelets (small cells that help the blood to clot), and plasma (the clear liquid part of blood, once cells are removed; it contains proteins) transfusions.
As a patient with CAD, you will most likely need a red blood cell transfusion.
Why would I need a transfusion?
The cold agglutinins that your body produces bind to red blood cells at colder temperatures. This causes the red blood cells to clump together, and are destroyed as they move through the body. Their loss often leads to anemia, a condition where your body doesn’t have enough red blood cells to carry oxygen at levels your tissues need. A red blood cell transfusion can replace lost red blood cells to help ease your symptoms.
How often do I need a blood transfusion?
A review study of 903 CAD patients, drawing on data spanning January 2007 to September 2018, reported that 39% of them (355 people) were treated with at least one transfusion, and most of them (297, 84%) went on to receive at least one more.
The American Association of Blood Banks (AABB) recommends that against a blood transfusion unless a person’s levels of hemoglobin (the molecules in red blood cells that carry oxygen) fall between 7 and 8 g/dL, or they have anemia-related complications. These guidelines aim to limit the risk of transfusion-related side effects.
How long does it take?
A transfusion of red blood cells usually takes between two and four hours.
How do I know what type of blood I need?
Generally, before you receive the blood transfusion, a sample of your blood will be tested to find your current red blood cell count, your level of cold agglutinin antibodies, and your blood type.
There are four main types of blood: O, A, B, and AB. In each type, there are specific proteins on the surface of red blood cells and antibodies in the plasma against the other proteins. All four blood types may or may not have Rhesus (Rh) factor proteins on the cell surface, making your blood either Rh-positive (+) or Rh-negative (-).
It is important to receive a compatible blood type so your immune system does not attack the donor blood.
Are there risks?
Blood transfusions are generally safe. However, there is a chance of rare complications. One of the more common is for you to have an allergic reaction to the transfusion, which can lead to fever, itching, and hives, during the transfusion or days later. Acetaminophen or antihistamines (allergy medicine) can help, as can slowing down the rate of the transfusion.
Your cold agglutinins could also bind to the new red blood cells. Warming the donor blood to body temperature before the transfusion can greatly reduce this risk.
A very low risk of contracting blood-borne diseases such as HIV, hepatitis, or Creutzfeldt-Jakob disease does exist. However, blood donors are screened, and donated blood is tested to ensure against such diseases before the transfusion.
Last updated: Feb. 4, 2021
***
Cold Agglutinin News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website.





